That tightness in your chest, that feeling of running out of breath with the slightest effort...
You're tired of that anxiety that creeps in with every wheezing breath.
Asthma can make you live in constant fear of the next attack.
You're looking for natural solutions, beyond inhalers, to reduce inflammation, relax your bronchi, and regain true respiratory peace.
Solutions like ginger, raw honey, or targeted breathing techniques exist and are backed by research.
In this article, we reveal a holistic 4-step protocol - understanding, identification, action, consolidation.
A clear action plan that combines herbs, dietary supplements, nutrition, and gentle therapies to help you regain control of your breathing.
🌿 Your Natural Asthma Protocol
4 steps based on herbs, diet, and natural techniques:
Step 1: Understand & Soothe
• Ginger: Relaxes respiratory tract muscles thanks to gingerol.
• Turmeric (with pepper): Reduces bronchial inflammation via curcumin.
• Raw honey (Manuka): Soothes nighttime cough and irritation.
Step 2: Identify & Nourish
• Omega-3 (fish/algae): Decreases production of inflammatory leukotrienes.
• Vitamin D3: Improves response to treatments and reduces flare-ups.
• Magnesium (bisglycinate): Relaxes bronchial smooth muscles.
Step 3: Act & Relieve
• Essential oils (Eucalyptus/Lavender): In inhalation, open bronchi and calm.
• Breathing exercises (Buteyko): Strengthen control and lung capacity.
• Acupressure (points LU7, CV17): Releases airways and reduces stress.
Step 4: Consolidate & Prevent
• Anti-inflammatory foods: Apples, spinach, pomegranates.
• Adapted activities: Swimming, Tai Chi to strengthen without triggering.
• Avoiding triggers: Dust mites, mold, mucus-producing foods.
How to use this guide:
If you're looking for quick relief during discomfort → Focus on Step 3 (essential oil inhalation, onion-honey syrup).
If you want to reduce attack frequency long-term → Follow the complete protocol, emphasizing Steps 2 (supplements) and 4 (prevention).
If your asthma is clearly linked to stress or allergies → Adopt techniques from Step 3 (breathing, acupressure) and identify your triggers in Step 4.
Step 1: UNDERSTAND – Target inflammation and bronchial contraction
Complementary natural approaches mainly target two asthma mechanisms: chronic bronchial inflammation and bronchial hyperreactivity (an excessive tendency to narrow).
Here are the most effective options you can try:
Ginger to relax respiratory tract muscles
Ginger contains interesting anti-inflammatory compounds like gingerol that specifically help relax respiratory tract muscles.
Studies show it can act like certain asthma medications by inhibiting airway contraction.
Practical protocol: Drink fresh ginger tea 2-3 times daily (steep 1 inch of grated ginger in hot water for 10 minutes).
Tip: Combine it with turmeric and black pepper for better absorption and a synergistic effect.
Turmeric to reduce lung inflammation
Curcumin, the active compound in turmeric, reduces airway inflammation by suppressing inflammatory cytokines.
Research indicates it can decrease asthma severity when taken regularly.
Optimal form: For maximum absorption, look for a curcumin supplement combined with piperine (black pepper extract), which improves absorption by 2000% (aff).
Studied dosage: 500mg twice daily with meals.
Raw honey to soothe cough and irritation
The antimicrobial and anti-inflammatory properties of honey soothe irritated airways and thin mucus.
Darker varieties, especially Manuka honey, are particularly promising.
Proven nighttime remedy: Take 1 teaspoon before bed to reduce nighttime coughing.
Essential safety precautions: Do not give to children under 1 year (risk of infant botulism).
Omega-3 fatty acids to modulate inflammation
EPA and DHA from fish oils reduce production of inflammatory leukotrienes, molecules that directly trigger asthma attacks.
Best food sources: Consume wild salmon, 3 servings weekly.
Supplement alternative: 1000mg fish oil daily (aff).
For vegetarians, an algae oil supplement is an effective option.
Step 2: IDENTIFY – Your profile and specific deficiencies
Recent research suggests certain supplements to relieve asthma can help manage symptoms when combined with standard treatment.
Identifying your potential deficiencies is a crucial step to personalize your natural anti-asthma protocol and target the most suitable dietary supplements for your case.
Questionnaire to identify your profile
"Inflammatory" Profile: Frequent attacks, persistent symptoms → Target Vitamin D, Omega-3, Turmeric.
"Allergic" Profile: Seasonal symptoms, triggered by dust mites and/or pollen → Target Quercetin, Probiotics, Vitamin C.
"Nervous" Profile: Attacks often triggered by stress or anxiety → Target Magnesium, breathing techniques, Lavender.
Vitamin D3: The essential immune regulator
A low vitamin D level is strongly associated with greater asthma severity.
Supplementation can reduce steroid-resistant asthma cases by 50% and decrease flare-up frequency.
Personalized dosage: 2000-5000 IU daily.
It's recommended to first test your blood level for precise adjustment.
Magnesium: The bronchial muscle relaxant
This essential mineral relaxes bronchial smooth muscles.
Studies show intravenous magnesium sulfate stops acute asthma attacks in emergency rooms.
In daily prevention: Oral magnesium at 300-400mg daily can reduce rescue medication needs.
Recommended form: Prefer magnesium glycinate for better absorption without digestive side effects (aff).
Vitamins C and E: The protective antioxidants
These antioxidants protect lung tissues from oxidative damage caused by inflammation and pollutants.
Vitamin C: 500-1000mg daily can reduce exercise-induced asthma.
Vitamin E: A mixed tocopherols blend at 400 IU daily helps decrease airway inflammation.
Quercetin: The natural mast cell stabilizer
This flavonoid is particularly interesting for allergic asthma, as it stabilizes mast cells that release histamine during allergic reactions.
Effective supplement dose: 500mg Quercetin twice daily, starting before allergy season.
Food sources: Onions, apples, capers.
Probiotics: For the gut-lung axis
Research on the gut-lung axis is promising.
Specific strains seem to modulate immune response:
- Lactobacillus rhamnosus may reduce the risk of developing asthma in children by 50%.
- Bifidobacterium longum appears to decrease airway inflammation.
General dosage: 10-20 billion CFU daily of a mixed probiotic strains blend.
⚠️ Important warning: Always consult a healthcare professional before starting any supplement, especially if you take blood thinners or other medications, to check for interactions.
Phytotherapeutic options
For those seeking to reduce dependence on corticosteroid inhalers under medical supervision, these natural options exist:
- Black seed oil (Nigella sativa): Contains anti-inflammatory thymoquinone (500mg twice daily reduces nighttime attacks by 42%)
- Boswellia serrata: Inhibits the 5-LOX enzyme (300mg three times daily)
- Pycnogenol: Maritime pine bark extract (reduces airway hyperreactivity)
Nutritional support
- Omega-3 index >8%: Reduces need for rescue inhalers
- Vitamin D >50 ng/ml: Makes steroids more effective
❗ Important warning: These alternatives should only be used:
- Under pulmonological supervision
- After restoring basic lung function
- While maintaining peak flow monitoring
Example transition protocol:
- Optimize vitamin D levels
- Introduce boswellia while reducing steroids by 25%
- Monitor symptoms weekly by keeping a journal

Step 3: ACT – Relieve quickly and strengthen daily
This step groups remedies and techniques you can implement to relieve respiratory discomfort, calm cough, or better manage your daily breathing.
How to stop an asthmatic cough at home?
These home remedies for asthmatic cough provide quick relief and are well-documented.
1. Steam inhalation with essential oils
Protocol: Add 3 drops Eucalyptus essential oil + 2 drops Lavender essential oil to a bowl of very hot water.
Method: Cover head with a towel and inhale steam for 5 minutes.
Effects: Opens airways and thins mucus for better expectoration.
2. Mullein tea
Protocol: Steep 1 teaspoon dried mullein leaves in a cup of hot water for 10 minutes.
Dosage: Drink this tea twice daily.
Benefits: This plant naturally soothes bronchial irritation and is traditionally used for respiratory issues.
3. Natural honey and onion syrup
Recipe: Layer onion slices and raw honey in a glass jar. Let rest overnight in a cool place.
Use : Take 1 teaspoon of the resulting syrup as needed to calm cough.
Clinical note: Comparative studies show this type of remedy can be as effective as dextromethorphan (a common cough suppressant) for suppressing cough.

Essential oils: safe usage protocols
When used safely, certain essential oils can provide complementary relief during asthma symptoms.
Top 3 emergency essential oils
Eucalyptus radiata: Opens bronchioles thanks to its main component, eucalyptol.
Application: 2 drops in shower steam or dry inhalation on a handkerchief.
Frankincense (Olibanum): Calms inflammation and may promote deeper breathing.
Application: Diffuse overnight in bedroom.
True Lavender: Reduces triggering by stress and anxiety.
Application: Apply 1 drop diluted in carrier oil on sternum or wrists.
Strict safety protocols (to follow)
⚠️ Never do:
- Apply undiluted essential oils to skin during an attack.
- Do not use peppermint oil on children under 6 years (risk of laryngeal spasm).
- Replace your rescue medications with essential oils.
✅ Do:
- First perform a skin test on the elbow crease to check for no reaction.
- Use a cold air diffuser (heat diffusers degrade oil properties).
- Combine their use with pursed-lip breathing for enhanced effect.
Clinical note : A 2021 study showed that eucalyptol (main compound in eucalyptus) reduces asthma exacerbations by 29% when used alongside standard care.
The best breathing exercises for asthma
Proper breathing techniques can significantly improve asthma control and lung function.
Diaphragmatic (or abdominal) breathing
- Lie on your back with knees slightly bent.
- Place one hand on chest, the other on abdomen.
- Breathe in deeply and slowly through nose for 4 seconds: hand on abdomen should rise, hand on chest moves little.
- Breathe out slowly and completely through mouth, with pursed lips as if whistling, for 8 seconds.
- Repeat this cycle for 5 to 10 minutes daily.
Documented results: A 2020 study showed a 40% reduction in rescue inhaler use after 8 weeks of regular practice.
Buteyko method
This method teaches controlled breath retention to normalize CO₂ levels in blood, which has a natural bronchodilator effect.
Simple initiation exercise:
- After a normal, passive exhale, gently pinch your nose.
- Gently hold your breath until feeling the first slight urge to breathe (no forced apnea).
- Release nose and resume calm, normal breathing through nose.
- Repeat this cycle 5 times, staying relaxed.

Step 4: CONSOLIDATE – Prevent attacks and optimize environment
This final step aims to create an environment and habits that support respiratory health long-term, by reducing exposure to triggers and strengthening the body.
Which foods help reduce asthma symptoms?
Nutrition plays a crucial role in asthma management.
Here is the best anti-inflammatory diet for asthma.
Top 5 foods against asthma
- Fatty fish (wild salmon, mackerel, sardines): Provide EPA/DHA that reduce inflammatory leukotriene production.
- Apples: Rich in quercetin and polyphenols protective of airways.
- Spinach: Excellent source of magnesium and folate, helping relax airways.
- Pomegranates: Their high punicalagin content helps reduce oxidative stress in lungs.
- Brazil nuts: Just 2 daily provide the daily dose of selenium, essential for boosting glutathione, a major antioxidant.
Coffee and asthma: an emergency tip
Caffeine has a mild bronchodilator effect, similar to theophylline medications sometimes prescribed.
Emergency tip : In case of a mild attack without immediate access to inhaler, 2 espressos can provide short-term relief while waiting for help or medication.
Foods to eliminate or test:
- Dairy: May increase mucus production in many asthmatics, though not an absolute rule.
- Processed meats: Often contain sulfites and nitrates, known potential triggers.
- Wheat/Gluten: May worsen inflammation in those with non-celiac sensitivity.
📌 Tip: Try a strict elimination diet for 4-6 weeks (no dairy, no gluten, no additives) to identify your personal triggers with certainty.
Is exercise good or bad for asthma?
Many asthmatics wonder if exercise helps or worsens their condition.
The answer is nuanced and strategic.
The exercise paradox explained
While exertion can trigger attacks (called exercise-induced bronchoconstriction), regular, adapted physical activity:
- Strengthens respiratory muscles (diaphragm, intercostals).
- Improves lung capacity and endurance.
- Reduces systemic low-grade inflammation.
Best exercises for asthma
→ Swimming
The warm, humid air of pools prevents airway drying, a major trigger.
The horizontal position helps eliminate mucus through drainage.
Ideal frequency: 30 minutes, 3 times weekly.
→ Tai Chi
This discipline combines deep breathing with gentle, fluid movements.
Studies confirm it can reduce rescue medication use.
→ Interval walking
Protocol: 2 minutes brisk walking followed by 1 minute slow recovery.
This method develops cardiovascular endurance without overworking lungs continuously.
Crucial precautions to respect:
- Always use your pre-exercise inhaler (bronchodilator) if prescribed, about 15 minutes before starting.
- In cold weather, wear a scarf or mask over mouth to warm and humidify inhaled air.
Stop activity immediately if:
- Wheezing that worsens.
- Persistent chest tightness.
- Dizziness or weakness.
Tip : The "15-minute rule"
Always include 15 minutes progressive warm-up (slow walking, stretching) before more intense activity to prevent exercise-induced attacks.

Which alternative therapies for asthma?
These alternative therapies for asthma management show scientific promise and can be integrated into your approach.
-
Acupuncture / Acupressure
Documented effect: May reduce IgE levels (allergy immunoglobulins) by 35% in allergic asthma.
Key points to stimulate:
LU7 (Lie Que): Located on Lung meridian, on wrist → Releases airways.
CV17 (Sea of Tranquility): At center of sternum → Calms mind and breathing.
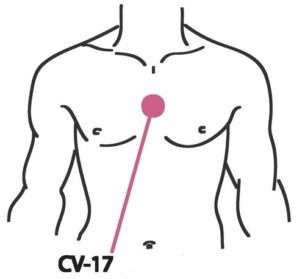
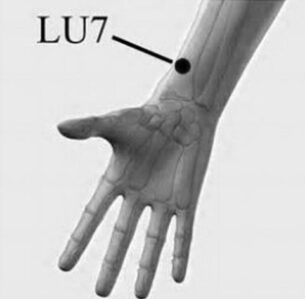
-
Chiropractic care
Principle: Correct spinal subluxations, particularly at dorsal level, that could affect lung and bronchial innervation.
Effectiveness: Often proves more effective when combined with specific breathing exercises.
-
Yoga therapy
Beneficial postures:
- Bridge Pose (Setu Bandhasana): Opens chest cavity and stretches respiratory muscles.
- Cobra Pose (Bhujangasana): Develops lung expansion capacity.
Results: Studies show 30% improved peak flow measured after 12 weeks of regular practice.
Which triggers to avoid when you have asthma?
Preventing exposure is the first step to natural asthma relief.
Major environmental triggers
- Dust mites: Use allergen-proof encasings for mattress and pillows. Wash bedding at 60°C.
- Mold: Maintain indoor humidity below 50% using dehumidifiers if needed.
Ventilate daily. - Pollen: Shower and wash hair in evening to remove accumulated pollen.
Keep windows closed during peak pollen periods.
Lifestyle-related triggers
- Stress and anxiety: Practice mindfulness meditation or heart coherence 10 minutes daily.
- Gastroesophageal reflux (GERD): Elevate head of bed 4-6 inches and avoid heavy evening meals.
- Sleep position: Elevating head to 30 degrees may help reduce nighttime symptoms and reflux.
⚠️ When to see a doctor for asthma?
Although natural solutions help, consult a doctor immediately or call 911 for:
Absolute emergency signs (respiratory distress)
- Bluish lips or fingernails (cyanosis, sign of severe oxygen lack).
- Inability to speak full sentences due to breathlessness.
- No improvement after 3 successive doses of your rescue inhaler (bronchodilator).
- Peak flow meter reading below 50% of your personal best.
Signs that baseline treatment adjustment is needed
- You wake up more than twice weekly with symptoms (cough, wheezing, tightness).
- You use your rescue inhaler more than twice weekly (aside from preventive use before exercise).
- Symptoms regularly interfere with your daily activities (climbing stairs, housework, etc.).
💊 The essential word on conventional treatments and safety
It's fundamental to remember that the natural approaches presented here aim to complement and optimize your medical care, never replace it.
Conventional asthma treatment (corticosteroid-based control inhalers and rescue bronchodilators) is prescribed for a precise reason: it controls underlying inflammation and prevents potentially severe attacks.
Our essential safety recommendations:
Never modify your treatment without medical advice: Any reduction in inhaled corticosteroid doses should be considered with your pulmonologist, based on objectively measured improvement (peak flow meter).
Your rescue inhaler remains your first reflex: At the start of an attack, use it immediately as prescribed.
Natural methods are preventive or supportive, not emergency solutions.
Caution with interactions: Certain supplements (high-dose vitamin E, ginger, omega-3) may thin blood.
Always report their use to your doctor, especially if you take blood thinners.
Regular follow-up is non-negotiable: Consultations with your doctor or pulmonologist and any lung function tests remain the cornerstone of good asthma control.
The ideal is a winning alliance: conventional medications to manage the disease, combined with validated natural strategies to reduce its symptoms, side effects, and improve your overall quality of life, under professional supervision.
Holistic approach to asthma management
Effectively managing asthma requires combining:
- Medical treatments (as prescribed)
- Natural solutions (ginger, honey, breathing exercises)
- Preventive strategies (avoiding triggers, supplements)
Key points to remember:
- Consistency matters: Most natural approaches take 4-6 weeks to show full effects
- Personalization is essential: Track symptoms to identify your unique triggers
- Professional guidance: Always work with your doctor when modifying treatment
By integrating these natural ways to improve lung function with conventional care, many achieve significant asthma relief and better quality of life.
Final tip: Keep an asthma journal to track what works best for your symptoms and triggers.
Your questions about living with asthma
Can asthma go away on its own?
While childhood asthma sometimes disappears in adolescence, adult asthma typically requires ongoing management. About 30% of children "outgrow" their asthma, but symptoms can reappear later.
Is asthma hereditary?
Yes, genetics play an important role. If one parent has asthma, a child has 25% risk; if both parents have it, risk rises to 50%. However, environmental factors often trigger genetic predispositions.
Can you develop asthma in adulthood?
Absolutely. Late-onset asthma affects about 1 in 12 adults, often triggered by:
- Hormonal changes (especially in women)
- Occupational exposures (chemicals, dust)
- Respiratory infections
- Stress or major life changes
Why does my asthma worsen at night?
Nocturnal asthma affects 75% of patients due to:
- Natural cortisol drop (increases inflammation)
- Lying position (mucus accumulates)
- Cooler bedroom air (triggers bronchospasms)
Solution: Use a humidifier and elevate head.
Can asthma permanently damage your lungs?
Poorly controlled asthma can lead to:
- Airway remodeling (permanent narrowing)
- Reduced lung function over time
- Increased risk of COPD
Prevention: Regular monitoring and appropriate treatment can prevent most damage.
How does weather affect asthma?
Each weather type can trigger asthma symptoms in specific ways:
- Cold/dry air: Causes airway constriction
- Humid weather: Promotes mold spore and dust mite proliferation
- Thunderstorms: Fragments pollen grains into finer, inhalable particles
- Strong winds: Disseminates allergens in air
- Air pollution: Worsens during thermal inversions
- Sudden temperature changes: Triggers bronchospasms
Practical advice: Check weather forecasts and pollen alerts to anticipate risky days.
* Last updated January 2026

